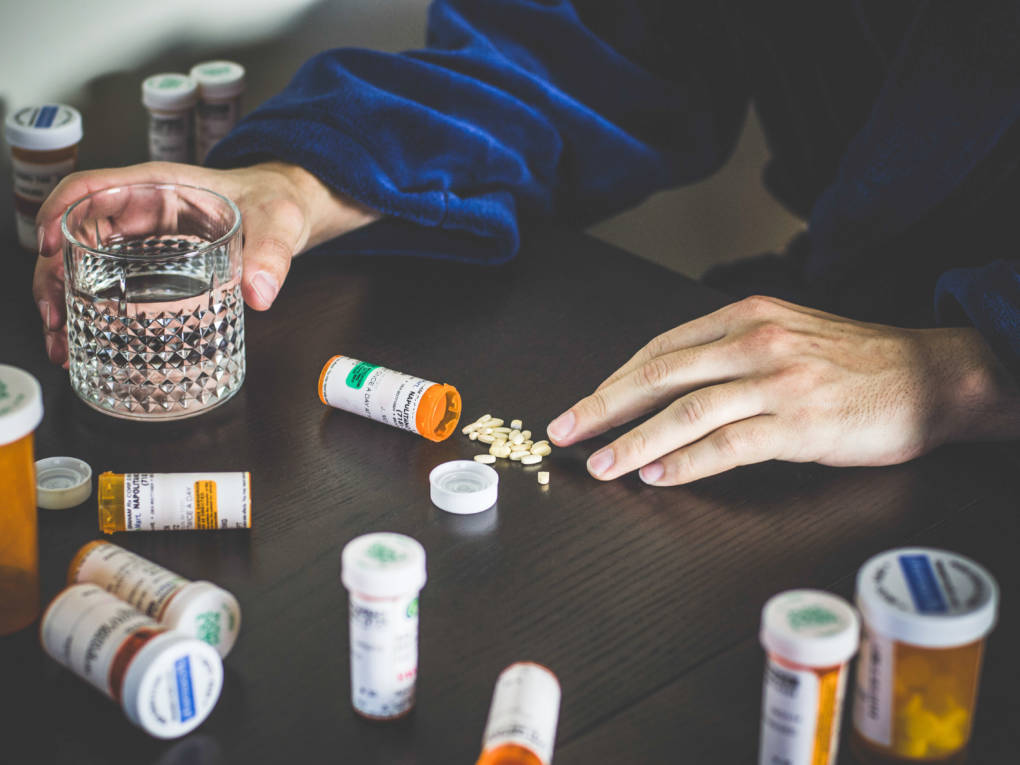
Medications should help fight disease, not harm the human body. To avoid the latter, it is important to strictly observe the frequency of intake, not to take more than the required dose, take into account the effect of food on absorption of a particular drug.
But the most important thing is to understand that some drugs should not be taken together, because they can interact with each other, changing each other’s therapeutic effect, in some cases negatively affecting the body.
What are drug interactions, what can they be
The term “drug interaction” is used to refer to situations in which the specific effects of at least one drug change significantly when two or more drugs are taken simultaneously. The risk of its occurrence is directly proportional to the number of drugs used: the more drugs enter the body together, the higher the probability of negative effects.
There are two main types of interactions:
- Pharmacodynamic (concerning the mechanism of action and the effect of the agent);
- Pharmacokinetic (affect the absorption, distribution, and excretion of drugs).
Pharmacodynamic interaction.
The administration of several drugs can cause two types of interactions related to their pharmacodynamics in the body:
- Synergism, which can manifest itself by potentiating the action of one drug or by summing up the effects of two drugs. For example, simultaneous administration of iron drugs with ascorbic acid increases their absorption and consequently increases their concentration in the blood. As an example of summation of the effects, we can give the interaction of two drugs from the group of non-steroidal anti-inflammatory pain relievers – paracetamol and acetylsalicylic acid (aspirin). Their simultaneous use can cause symptoms similar to an overdose: dizziness, disorientation, nausea, diarrhea, bleeding in the gastrointestinal organs.
- Antagonism is a type of interaction in which one drug eliminates the effect of a second drug. Leads to the complete disappearance of the therapeutic effect of the drug or to its weakening. In some situations, antagonism can be a useful type of interaction, such as when antidotes are needed. But in most cases, inappropriate prescribing of several drugs with antagonistic effects to each other leads to ineffective treatment. A striking example of antagonism is the neutralization of sulfonamide drugs (e.g., streptocide, biseptol, sulfadimesin, phthalazole) by para-aminobenzoic acid (B vitamins, novocaine, dicaine, procaine, benzocaine). Their simultaneous administration leads to a significant decrease in the antimicrobial properties of such drugs.
Pharmacokinetic interaction
Some drugs cannot be taken together not only because of changes in their therapeutic effect, but also because of pharmacokinetic interaction. Both absorption and transport, metabolism, distribution and even excretion of one or both drugs, i.e. all the processes that take place with a drug after it enters the body, can change.
The end result of such transformations can be a change in the concentration of the active substance in the body, which is the key to treatment.
What can happen if possible pharmacokinetic interactions are not considered:
- A change in the motility of the gastrointestinal tract, resulting in different absorption of some drugs. For example, taking laxatives reduces the absorption of the drug. Cholinolytics, prokinetics and anticholinesterase agents – increase its absorption;
- Decrease or increase gastric acidity, resulting in altered absorption of the active ingredient of some drugs. There are drugs that require an acidic environment for complete absorption and to reach a certain concentration in the body. There are also drugs that require an alkaline pH, so you need to consider the possible change in acidity under their action. For example, if antacids are prescribed, you should not take them together with antiviral drugs: zalcibatin or tipranavir. Exactly for these drugs you need a low pH, otherwise absorption will be slowed down;
- Competitive binding to plasma proteins, which leads to an increase in the blood concentration of one of the drugs. This mechanism is explained by the fact that some drugs bind to plasma proteins by 90-98%, and when a patient takes simultaneously with them drugs that have a high degree of similarity to the same proteins, the former are displaced by the latter. One example: the antiarrhythmic drug quinidine can displace digoxin. Due to this, the concentration of digoxin in blood increases, as if the patient took a dose several times larger than usual. This leads to unpleasant symptoms and increased side effects: nausea, vomiting, headache, decreased pulse, dizziness;
- Changes in cytochrome P-450 activity. At its increase, a decrease in drug concentration and insufficient treatment efficacy are observed, while at a decrease in activity – on the contrary. For example, antifungal drugs (ketoconazole, fluconazole), antibiotics (erythromycin, clarithromycin) are inhibitors of enzyme activity. Examples of inducers are carbamazepine, ritonavir, rifabutin and others.
Unwanted and dangerous drug “couples”
Drug interactions are commonly divided into four classes:
- A – this class includes combinations in which the interaction is not clinically significant (for example, the combination of phenobarbital and ranitidine);
- B – this class includes pairs of drugs whose interactions have not yet been described
- C – a class of interacting drugs that change each other’s therapeutic effect. Can be eliminated by adjusting the dosage (cimetidine and theophylline)
- D – this class includes pairs of drugs, the reception of which at the same time can be dangerous and unacceptable.It is about such combinations and it is worth talking about.
Contraceptive hormones and antibiotics
To prevent an unplanned pregnancy, a doctor may prescribe oral contraceptives to a woman. These are hormonal drugs whose mechanism of action is based on suppression of ovulation. So even if the most “active” sperm get into the cervix, fertilization will not happen, because the egg does not mature.
Antibiotics, on the other hand, can be part of the treatment regimen for infectious diseases. They kill the bacteria, but also “kill” the beneficial microflora. It is this side effect of antibiotics that causes the decrease of hormones in the body. Because of the disruption of microflora in the gut, the hormones are practically not absorbed, and therefore stop working. As a result, a woman may become pregnant if she does not take additional precautions. Such a combination of drugs is not dangerous for the body, but if pregnancy is not planned, it must be taken into account.
Anticoagulants and analgesics
Drugs in the anticoagulant group are used to thin the blood and prevent thrombosis. The main danger of overdose of such drugs is the occurrence of internal bleeding.
Analgesic drugs have a very different purpose and mechanism of action. They relieve pain of different origin, but their additional effect is to reduce blood clotting. For this reason, the simultaneous use of these two groups of drugs can lead to bleeding in the internal organs. Such a condition is dangerous primarily due to blood loss. It is important not to abuse painkillers while continuously taking anticoagulants or to discontinue their use, if possible, for the duration of therapy with drugs from the NSAID group.
Calcium channel blockers and beta blockers
Medications that refer to calcium blockers are designed to treat arterial hypertension and angina pectoris. They act by blocking the calcium that constricts blood vessels, thereby dilating them. This lowers blood pressure and makes the blood flow to the heart work better. At the same time, calcium channel blockers affect the heart itself, so bradycardia and intracardiac blockages are possible when using them.
Beta blockers are used for coronary heart disease, arrhythmias, arterial hypertension, and chronic heart failure. They reduce heart rate and cardiac conduction. The superposition of such effects from two drugs at once can cause sudden cardiac arrest. If beta-blockers and calcium channel blockers are prescribed at the same time, the heart rate should be monitored carefully. In case of serious bradycardia – less than 50 beats per minute, you should immediately consult a doctor.
Anti-allergy and anti-cold medications

At the first symptoms of a cold, many people choose sachets of powder to make a hot drink. They are really quite good at coping with headache, body aches, nasal congestion. And all because the composition is paracetamol, as well as antihistamine components. If you combine these sachets with drugs for allergies, you can face an overdose of the latter. As a result – high drowsiness, which is very dangerous for drivers or those who work with mechanisms that require concentration.
Exactly the same danger is posed by mixing antihistamines with motion sickness and seasickness remedies.
Antidiarrheals and calcium preparations
The dangerous combination of these two groups of drugs concerns primarily loperamide-based diarrhea remedies. Such a drug reduces intestinal motility, thereby reducing the frequency of defecation. It should not be taken for intestinal infections, because pathogenic microflora will not be eliminated from the body, which will lead to an increase in intoxication.
Calcium is a mineral that helps strengthen bones. It is often prescribed for fractures and to prevent osteoporosis in menopausal women. Calcium can also be a part of remedies to reduce the acidity of gastric juice. In addition to strengthening bone tissue, it also affects intestinal motility, just like loperamide. The simultaneous use of these two drugs can lead to prolonged constipation. This is why you should avoid calcium products during the treatment of diarrhea with loperamide.
Antifungal agents and statins
Medications from the statin group are used to lower cholesterol and prevent atherosclerosis. They disrupt the process of cholesterol production by the liver, so it “takes over” the processing of what is already in the blood. Such drugs are often prescribed in the complex therapy of arterial hypertension. Antifungal agents are used to treat dermatomycosis, oral candidiasis, vaginal candidiasis, onychomycosis.
The cytochrome P-450 enzyme takes part in the metabolism of both drugs, so simultaneous administration of antifungals and statins can lead to increased levels of the latter in the blood and their accumulation in the skeletal muscles. The result of this penetration of cholesterol-lowering agents is a high risk of developing rhabdomyolysis.
Also, you should not take statins together with anticoagulants because bleeding may occur.
ACE inhibitors and spironolactone
ACE inhibitors are a fairly popular group of drugs for the treatment of arterial hypertension.
Their mechanism of action is based on blocking the production of angiotensin, which constricts blood vessels. Thus, the blood vessels dilate and the blood pressure decreases.
Spironolactone is the active ingredient in medications prescribed for heart failure. It reduces blood volume by removing excess fluid and salts, thereby reducing the strain on the heart.
Both drugs increase blood potassium levels, which can lead to hyperkalemia. The danger of this condition is that heart rhythm and conduction are affected.
How to avoid negative effects on the body
The most important rule to avoid dangerous effects from taking two or more medications at the same time is not to self-medicate.
It is better to entrust the prescription of drugs to doctors. It is in this case you can get the maximum benefit from the treatment. In the extreme case, you need to carefully study the instructions to know what you should take the drug with, and what is strictly prohibited.
The second thing that every patient should remember is that it is important to strictly observe the dosage and time intervals. If there is a need to take two or more medications, it is advisable to take them separately. The minimum interval between different medications should be 30 minutes.
And the last thing – when undergoing treatment simultaneously by several specialists, it is necessary to warn them about all the drugs prescribed, otherwise you may encounter an unforeseen or even dangerous to your health result of such therapy.
Sources
- Wikipedia. – The relationship of liquids.
- Pharmaceutical Encyclopedia. – The interrelationship of drugs.
- Drug Interactions: What You Should Know
- Drug Interactions Checker
Read also:
- How do I check my gastrointestinal function?Stomach pain, constipation or diarrhea, bloating, belching, heartburn? These are all symptoms of problems in the gastrointestinal tract. It starts with the mouth and esophagus and ends with the intestines and rectum.
- What are the benefits of hazelnut oil for the skin?Hazelnut oil is rich in vitamins and essential fatty acids that nourish the skin. Here are a few reasons why you should add this oil to your skin care routine.
- Immune-boosting aromatic oilsThere are many products and treatments that can help your body to build a natural resistance to the harsh winter months, and aromatherapy is one of them. There are many studies supporting the healing power of aromatherapy and it is good for both mental and physical health. Aromatic essential oils also have many health benefits… Read more: Immune-boosting aromatic oils
- Marula Oil Benefits, Uses, and PrecautionsMarula Oil is an exotic oil that comes from the African Marula tree. It’s a good ingredient for skin, hair, and nails. Learn more about the benefits and precautions of Marula Oil with our guide.
- Goal setting for students, children and young peopleRemember when you learned how to set goals? If you have trouble answering this question, you are not alone! Most of us don’t spend much time thinking about how we set our goals. In fact, many of us don’t even think of goal setting as a skill; rather, it’s something we do without much thought.… Read more: Goal setting for students, children and young people
The articles on this site are for information purposes only. The site administrators are not responsible for attempting to apply any recipe, advice or diet, nor do they guarantee that the information provided will help or harm you personally. Be cautious and always consult a doctor or nutritionist!
*All products recommended are selected by our editorial team. Some of our articles include affiliate links. If you buy something through one of these links, you help us earn a small commission from the seller and thus support the writing of useful and quality articles.